What Is Flatfoot? 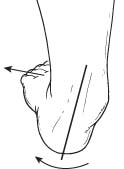
Flatfoot is often a complex disorder, with diverse symptoms and varying degrees of deformity and disability. There are several types of flatfoot, all of which have one characteristic in common: partial or total collapse (loss) of the arch. Other characteristics shared by most types of flatfoot include toe drift, in which the toes and front part of the foot point outward. The heel tilts toward the outside and the ankle appears to turn in. A tight Achilles tendon, which causes the heel to lift off the ground earlier when walking and may make the problem worse, bunions and hammertoes may develop as a result of a flatfoot.
Flexible Flatfoot
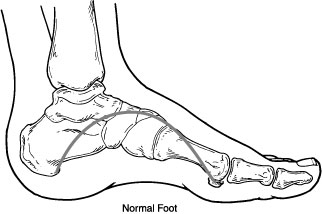 Flexible flatfoot is one of the most common types of flatfoot. It typically begins in childhood or adolescence and continues into adulthood. It usually occurs in both feet and progresses in severity throughout the adult years. As the deformity worsens, the soft tissues (tendons and ligaments) of the arch may stretch or tear and can become inflamed. The term “flexible” means that while the foot is flat when standing (weightbearing), the arch returns when not standing.
Flexible flatfoot is one of the most common types of flatfoot. It typically begins in childhood or adolescence and continues into adulthood. It usually occurs in both feet and progresses in severity throughout the adult years. As the deformity worsens, the soft tissues (tendons and ligaments) of the arch may stretch or tear and can become inflamed. The term “flexible” means that while the foot is flat when standing (weightbearing), the arch returns when not standing.
Symptoms
Symptoms that may occur in some persons with flexible flatfoot include:
- Pain in the heel, arch, ankle or along the outside of the foot
- Rolled-in ankle (overpronation)
- Pain along the shin bone (shin splint)
- General aching or fatigue in the foot or leg
- Low back, hip or knee pain
Diagnosis
In diagnosing flatfoot, the foot and ankle surgeon examines the foot and observes how it looks when you stand and sit. X-rays are usually taken to determine the disorder’s severity. If you are diagnosed with flexible flatfoot, but you do not have any symptoms, your surgeon will explain what you might expect in the future.
Nonsurgical Treatment
If you experience symptoms with flexible flatfoot, the surgeon may recommend nonsurgical treatment options, including:
- Activity modifications. Cut down on activities that bring you pain and avoid prolonged walking and standing to give your arches a rest.
- Weight loss. If you are overweight, try to lose weight. Putting too much weight on your arches may aggravate your symptoms.
- Orthotic devices. Your foot and ankle surgeon can provide you with custom orthotic devices for your shoes to give more support to the arches.
- Immobilization. In some cases, it may be necessary to use a walking cast or to completely avoid weightbearing.
- Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, help reduce pain and inflammation.
- Physical therapy. Ultrasound therapy or other physical therapy modalities may be used to provide temporary relief.
- Shoe modifications. Wearing shoes that support the arches is important for anyone who has flatfoot.
- Ankle Foot Orthoses (AFO) devices. Your foot and ankle surgeon may recommend advanced bracing to modify your walking and to support your arches.
When Is Surgery Necessary?
In some patients whose pain is not adequately relieved by other treatments, surgery may be considered. Many surgical techniques are available to correct flexible flatfoot, and one or a combination of procedures may be required to relieve the symptoms and improve foot function. In selecting the procedure or combination of procedures for your particular case, the foot and ankle surgeon will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level and other factors. The length of the recovery period will vary depending on the procedure or procedures performed.